Using TMS to Augment and Treat Substance Use Disorders
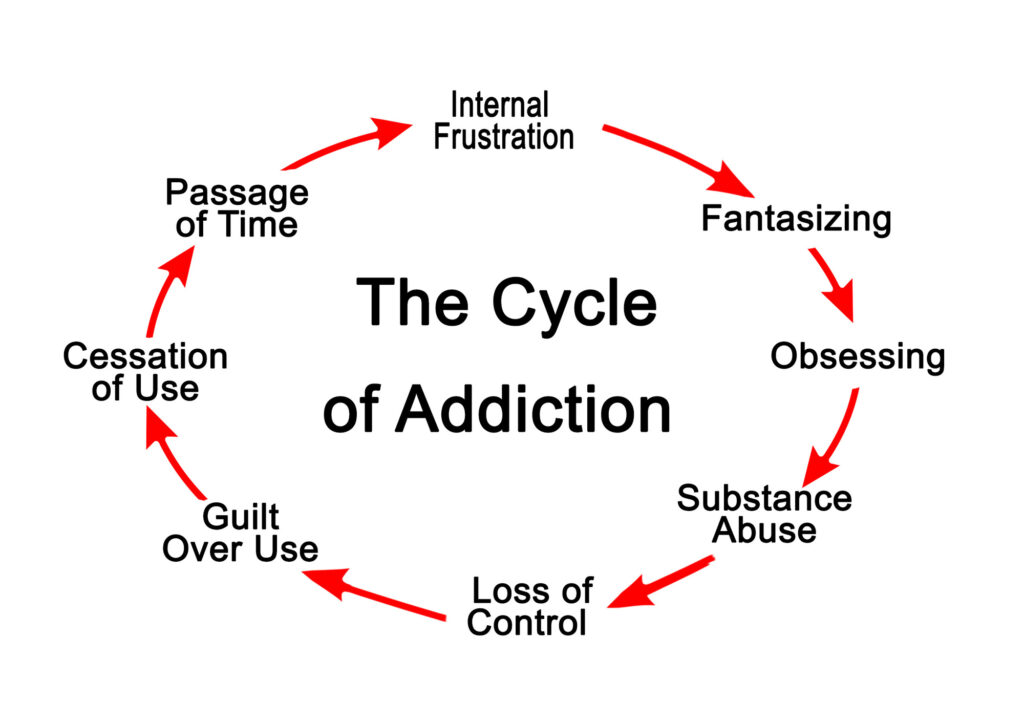
Could transcranial magnetic stimulation be the difference between life and death for those afflicted with a substance use disorder or addiction?
In this article you will learn why so many people with substance use disorders and addiction struggle to overcome the vicious cycle in their life. Additionally, we’ll discuss how TMS therapy may be the most viable treatment option to use as an adjunct to other treatment modalities or a primary treatment option for those who find it difficult to commit and maintain compliance with other therapies.
Substance use disorders (SUD) create a major impact on an individuals social functioning, and physical and mental health. They also create a huge burden on families and society as a whole, and contribute to worsening disease processes, accidents, mortality, and higher rates of suicidality – all of which are a negative impact on society. Can transcranial magnetic stimulation (TMS) help those with SUDs and assist in negating the societal burden?
SUDs occur from changes in the brain that result from repeated use of alcohol or drugs. Therefore, long-term substance use can significantly affect how brain circuits work. The most severe expression of a SUD is addiction. This change in brain circuitry can cause changes in the areas of the brain the affects ‘pleasure’ (the brains reward system), learning, stress, decision-making, and self-control. While all substances have a different effect on the brain, all addictive substances, such as alcohol, opioids, and cocaine produce an influx of dopamine in an area of the brain called the basal ganglia. Dopamine is a neurotransmitter. Neurotransmitters are brain chemicals that carry messages between nerve cells in the brain. The basal ganglia is an area of the brain that is our ‘reward center’ that controls reward and our ability to respond and learn based on rewards. So, as a person continues to use substances, these brain circuits adapt and learn from repeated use. In turn, their sensitivity to dopamine is reduced. When this occurs, eventually the substance no longer produces a ‘high’ and the individual builds up a tolerance.
Sadly, as the SUD progresses and individuals begin to increase daily use in an effort to chase the ‘high’, the pleasure that life has to offer, such as family, social interaction, food, and intimacy begins to fade. Eventually, the brain is re-trained to associate the high with other rewarding triggers associated with the SUD or addiction. These triggers are what can make efforts to quit so difficult. Ultimately, life beyond the substance is no longer enjoyable.
Substance use disorders and addiction also has a significant impact on the amygdala and prefrontal cortex areas of the brain too. The extended amygdala is responsible for how we react to stress. Over time, a person with a SUD may likely feel emotional and physical distress, especially when not able to get the drug. The physical distress often causes debilitating symptoms, such as nausea, weakness, vomiting, tremors, muscle aches and spasms, sweating, and difficulty sleeping. This distress can be quite difficult as the hours without use go by and triggers the body to withdrawal. However because it can be so difficult to endure, most people relapse in a short period of time. Therefore, a viscous cycle ensues, and the individual ends up deepening the wound with each repeated relapse. This repeated use helps to avoid the horrific feelings of irritability, depression, anxiousness, and physical symptoms when not using or drinking.
Treatment for SUDs and addiction
Substance use disorders and addiction can be extremely difficult to treat and everyone responds to the limited available treatments differently. Presently, the most effective treatment typically requires a long-term rehabilitation stay away from triggers and the ability to relapse. For a small percentage of people, an inpatient detoxification followed by intensive outpatient therapy or rehabilitation can work along with strong family support and financial resources, such as insurance coverage or the ability to afford treatment. However, many people with SUDs do not have insurance or the financial resources to get the help they need.
For others, they are prescribed medications to assist with relapse prevention. The use of medications in the treatment of SUDs can play a major role in preventing relapse and facilitating longer periods of abstinence. However, these medications are intended to be used as an adjunct to outpatient therapy, psychotherapy, and an overall treatment plan – although they are often prescribed to individuals without the other pieces of the treatment puzzle taking place. Medications used in the presence of SUDs or addiction offer three objectives: 1) management of the acute withdrawal period through detoxification, 2) reduction of cravings and urges during initial recovery, and 3) prevention of relapse to compulsive drug use. Agonist medications (those that attach to the same receptors in the brain as the drug) are also often prescribed for treatment retention and to reduce harm. However, these are often abused as well.
Regenerating new circuitry in an addicted brain with TMS
Transcranial magnetic stimulation (TMS) is used to treat a wide variety of clinical diagnoses. Predominately, TMS is used to treat major depressive disorder (MDD). However, this is because it was first FDA-approved for MDD and has been covered by insurance since 2014. TMS is used to regenerate neurotransmitters in a specific area of the brain. This area of the brain affected by MDD and treated with TMS is called the left dorsolateral prefrontal cortex. As with medication, TMS is used off-label (non-FDA approved) to treat other neurological, mental, and behavioral health conditions, such as bipolar depression, anxiety disorders, certain types of dementia, and substance use disorders.
Despite considerable advances in understanding the neural physiology of SUDs, treatment options remain limited. However, much research has highlighted the benefits of repetitive transcranial magnetic stimulation (rTMS) as a potential effective, safe, and cost-effective treatment option for certain SUDs. To date, we know that illicit substances, such as cocaine, modify to strength of connections between neurons (cells) in the brain. TMS works to improve neuroplasticity in the brain. Neuroplasticity is the process where neuronal synapses (connections between brain cells), become altered. This occurs as a result of behavioral, environmental, and the neural changes that occur over time (as discussed above).
When a person is treated with rTMS, it produces long-term neurophysiological changes that are induced by repetitive stimulations applied by an electromagnetic coil placed on the head to target a specific area of the brain. As TMS targets the damaged areas of the brain for an extended period, research shows long-term benefits and an increase in neuronal pathway regeneration and connections. This can have a significant impact on the cycling behaviors related to those with SUD who are repeatedly challenged by cravings and relapse.
In conclusion, while healthy adults are able to control impulses that are balanced by the judgment and decision-making circuits of the prefrontal cortex, unfortunately, these circuits are disrupted in those with SUDs. rTMS used alone or as augment to other treatment modalities could make a significant impact on the effectiveness of treatment for those afflicted with a SUD or addiction. Moreover, rTMS could mean the difference between life and death for a number of individuals currently living with a SUD or addicted brain. Help make a difference in another’s life.
Find a TMS therapy clinic in your area and seek treatment today.